March 23, 2017
Anita Svadzian, MPH and Prof. Madhukar Pai, MD, PhD
On 27 February, the WHO published a list of antibiotic-resistant “priority pathogens.” The first of its kind, this list is intended to promote research, discovery and development (R&D) of new antibiotics, as part of WHO’s efforts to address the threat of antimicrobial resistance (AMR) and respond to an urgent public health need. The hope is that the list will catalyse governments to incentivize basic science and advanced R&D.
The WHO list had one glaring and controversial omission – tuberculosis (TB). Prepared for an obvious backlash from the TB community against this “oversight,” the authors defended their decision, contending that TB is already a globally established priority and that it is clear to the world that innovative new treatments are urgently needed.
As predicted, an immediate response of outrage and total dismay from the TB community ensued. The Stop TB Partnership stated that the list presents “significant implications for the manner in which we will fight TB and drug resistant TB as it widely acknowledged the numerous gaps in implementation, research and innovation to rapidly detect, treat, and cure persons afflicted with drug resistant TB.” The Union (International Union Against Tuberculosis and Lung Disease) stated that it is “outrageous to sideline TB from global antimicrobial resistance (AMR) efforts” and added that the WHO must revise the list to include TB.
In response, the WHO quickly sent out a press release to reiterate the urgency for R&D of new antibiotics to address growing global burden of drug-resistant tuberculosis (DR-TB). Further clarification of the scope of the document explained that the prioritization exercise targeted hitherto unrecognized antibiotic-resistant pathogens. Accordingly, the WHO stressed the imminent need for R&D for DR-TB in tandem with the newly-prioritized pathogens.
Despite this attempt to smooth the waters and rationalize the exclusion, the Hashtag #TBontheList was born and the Stop TB Partnerships wrote an open letter to the WHO to put #TBontheList. Thomas Frieden, former director of the US CDC, sent a strong message via social media by tweeting: “TB is #1 infectious killer. Either 1. WHO list of priority research is pointless, or 2. WHO should fix it.”
Regardless of the confusion created by WHO, and the missed opportunity to include TB in an important advocacy effort, it is critical to recognize that drug-resistant TB is a key aspect of the global AMR crisis. In 2015, there were an estimated 480 000 new cases of multidrug-resistant TB (MDR-TB) and only 125 000 (20%) of these were enrolled in treatment. Only about half of patients treated for MDR-TB globally are cured, and the results are substantially worse for extensively drug-resistant disease (XDR-TB).
The harsh and surprising reality is that most of the drugs used for treatment of resistant strains of TB are antiquated and the need for innovation is dire. With most antibiotics used for treating TB invented before astronauts walked on the moon, health care workers and patients alike are struggling to make do with what is made available to them. Only two new TB medicines have been approved since this time. Even so, though bedaquiline and delamanid were approved in 2012 and 2014, respectively, access has been extremely restricted. Patient such as Tiong Xun Ting, Deepti Chavan, Nandita Venkatesan, Saurabh Rane, Phumeza Tisile offer moving testimonies of their personal battles with DR-TB and highlight the toxic and devastating nature of the treatments currently available, and the desperate need for new drugs and tools in the battle against drug-resistant TB.
In conclusion, DR-TB should be a critical component of the global response to AMR. The TB community needs to build on the momentum gained by an all-inclusive response to AMR and piggyback off the attention AMR gets as a focal issue for the global health security agenda by policy makers and donor agencies. As the world’s most influential health agency, if the WHO does not prioritize research for TB as part of a collective effort against AMR, even the small store of political will that exists to support TB R&D will dwindle. As many of our colleagues have already done, we urge WHO to publish a revised list, with TB in its rightful spot.
________________________
Anita Svadzian, MPH, completed her MPH in Epidemiology at Boston University, and will begin her PhD (Epidemiology) training at McGill University, Montreal, and the McGill International TB Center in September 2017. She is currently working on various projects through McGill’s agreement with UNOPS – Stop TB Partnership – TB REACH. She is extremely interested in the social determinants of health and understanding the interdisciplinary dynamics of health research. Twitter: @svadzianita
Prof Madhukar Pai, MD, PhD is a Canada Research Chair in Epidemiology & Global Health at McGill University, Montreal. He is the Director of McGill Global Health Programs, and Associate Director of the McGill International TB Centre. He serves as a Consultant to the Bill & Melinda Gates Foundation. He serves on the STAG-TB committee of WHO, Geneva; Scientific Advisory Committee of FIND, Geneva; and Access Advisory Committee of TB Alliance, New York. Twitter: @paimadhu
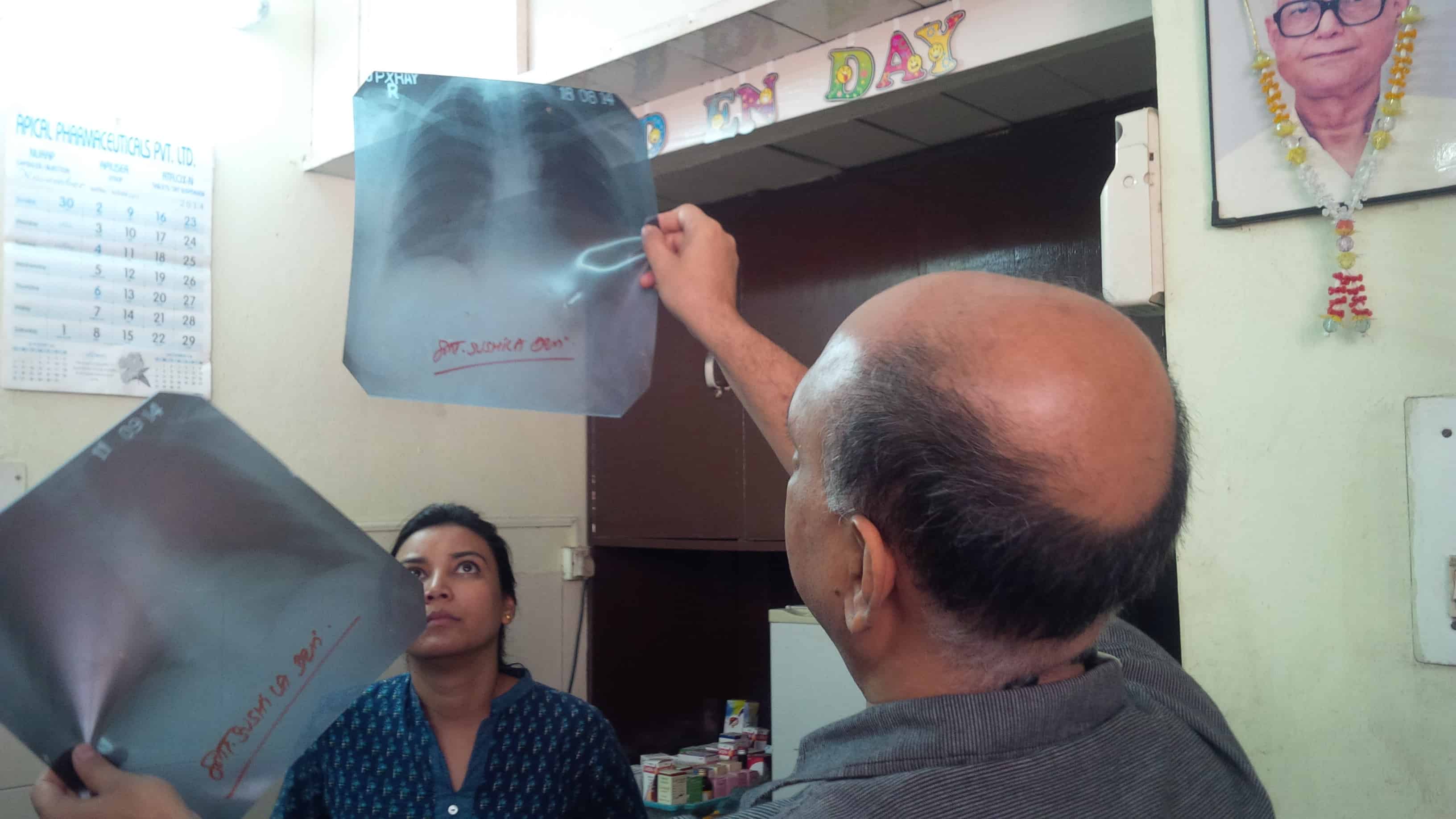
Image courtesy of Madhukar Pai