December 12, 2019

Funding gaps slow global malaria progress. According to the World Health Organization’s World Malaria Report 2019, there were 228 million cases and 405,000 malaria deaths last year, most of which occurred in sub-Saharan Africa. Global malaria rates remained stagnant between 2014 and 2018, and the report notes funding gaps as a barrier to progress. Although progress has stalled, the number of pregnant women and children who were engaging in prevention behaviors, including the use of mosquito nets and prevention medication, increased significantly between 2017 and 2018. [WHO]
Over 140,000 people died from measles in 2018. The World Health Organization (WHO) and the US Centers for Disease Control and Prevention (CDC) estimate that over 140,000 people died from measles in 2018. Measles death disproportionately affects children under 5 and this burden is high in Sub-Saharan Africa. The global measles vaccination rate is only 70 percent for the second dose of the vaccine, whereas 95 percent coverage is recommended to prevent outbreaks and to protect vulnerable populations from the virus. In 2018, Albania, Czechia, Greece and the United Kingdom lost their measles elimination status, and the United States reported the highest number of measles cases in 25 years. [WHO]
European countries are failing to report WHO’s 12 priority pathogens. Researchers assessed the mandatory reporting of the World Health Organization’s (WHO) 12 antibiotic-resistant priority pathogens across Europe in 2017 and found that only two-thirds of countries mandated surveillance of at least one pathogen. Among the 15 countries that had publicly available surveillance systems, 38 percent reported Carbapenem-resistant Enterobacteriales, 38 percent reported methicillin-resistant Staphylococcus aureus, and 25 percent reported vancomycin-resistant enterococci. None of the countries included in the study required reporting of antibiotic resistant Salmonella, Campylobacter, Helicobacter pylori, or Neisseria gonorrhoeae. [Clinical Microbiology and Infection]
Global preclinical antibiotic pipeline holds promise. In a review on the global preclinical pipeline of antibacterials in development, antibiotic resistance experts found that as of May 2019, 314 institutions were working on a total of 407 antibacterial projects. A majority of the projects focus on Gram-negative bacteria from the World Health Organization’s priority pathogen list, and many projects are taking unique approaches to overcome antibiotic resistance, including the use of probiotics and engineered phages. While the scope of the preclinical pipeline is more promising than that of the current clinical pipeline, the review notes that more work and funding are needed to bring effective therapies to the market. [Nature Reviews Microbiology]
New MRSA diagnostic test may improve infection prevention and control. The US Food and Drug Administration (FDA) approved a diagnostic test that detects the colonization of methicillin-resistant Staphylococcus aureus (MRSA) from nasal swabs using bacteriophage technology. The new test speeds up the diagnosis process, allowing health workers to identify MRSA colonization in as little as 5 hours, compared to 24-48 hours, which may improve prevention and control of the pathogen. [FDA]
Gavi funds malaria vaccine pilot program through 2023. Gavi, the Vaccine Alliance, has pledged an additional $11.6 million in support of the RTS,S malaria vaccine program from 2021 to 2023. The pilot program, which aims to vaccinate nearly 360,000 children each year, was first introduced in Ghana, Malawi, and Kenya this year to evaluate the safety and efficacy of routine use of the malaria vaccine. [Gavi]
Gavi programs linked to increased global immunization rates and decreased child mortality. In a quasi-experimental study, researchers found that Gavi funding programs have increased diphtheria, pertussis and tetanus (DPT) and measles vaccination coverage by 12.02 and 8.81 percentage points respectively between 1995 and 2016. Gavi support was also associated with a decrease in infant and under-five death rates during the study period (rates decreased by 6.22 and 12.23 deaths per 1000 live births). [BMJ Global Health]
Vaccine reduces incidence of typhoid fever among Nepalese children in clinical trial. In a phase 3 trial of more than 20,000 children in Nepal, one dose of a typhoid conjugate vaccine effectively reduced the incidence of typhoid fever compared to a meningococcal conjugate vaccine (79 vs. 428 cases per 100,000 person-years; Vaccine efficacy: 81.6 percent). Rates of adverse events occurred similarly across trial groups, and seroconversion occurred in 99 percent of children in the typhoid conjugate vaccine group, compared to only 2 percent in the control group. [NEJM]
Biomarker-guided stewardship ineffective at reducing antibiotic use in patients with suspected ventilator-associated pneumonia. In a randomized controlled trial across England, Scotland, and Northern Ireland, researchers found that biomarker-guided antibiotic stewardship was not effective at reducing antibiotic use among patients with suspected ventilator-associated pneumonia. The study found no significant difference between antibiotic-free days in the intervention and control groups in the week following the biomarker test (p=0.58). The authors suggest that prescribing culture may be driving antibiotic use among patients. [The Lancet Respiratory Medicine]
Maternal and child health clinics serve as a platform for PrEP delivery in Kenya. In a study of 9,376 pregnant and post-partum women across Kisumu County, Kenya, researchers evaluated maternal and child health clinics as a platform for HIV pre-exposure prophylaxis (PrEP) delivery for women. PrEP initiation was more likely among women who had a partner who was living with HIV, women who had previously been diagnosed with a sexually transmitted infection, and those who had been forced to engage in sex (adjusted prevalence ratio=6.96, 1.57, 1.82), among other factors. Of the 2,030 women who initiated PrEP use, 68 percent of those with an HIV-positive partner continued use after one month compared to only 38.7 percent of women overall. Women reported side effects and low HIV perception as factors that led to PrEP discontinuation. [The Lancet HIV]
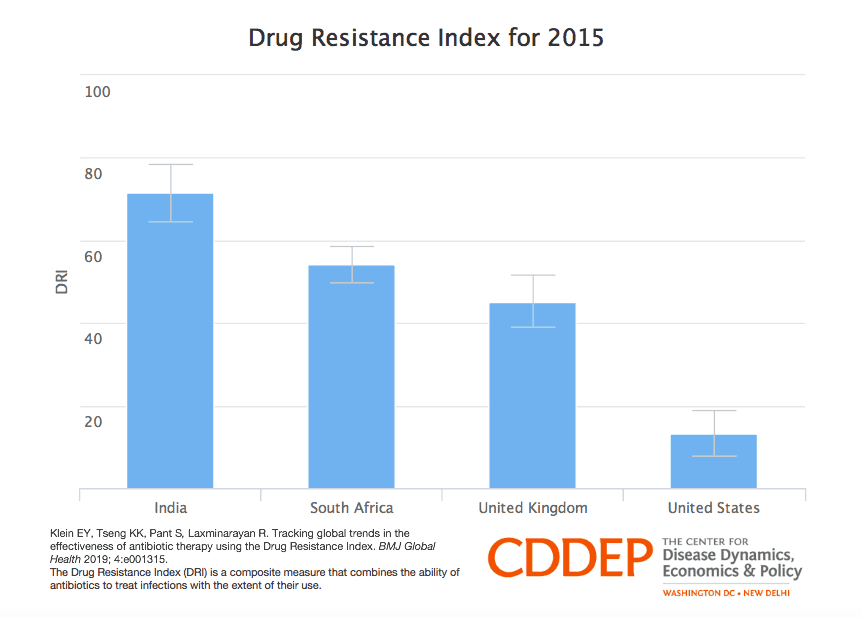
Comparing the Drug Resistance Index across India, South Africa, UK, and US. [CDDEP]