March 23, 2018
India’s ambitious goal: Eradicate TB by 2025. In advance of World TB Day on March 24, 2018, Indian Prime Minister Narendra Modi announced India’s plans to eradicate tuberculosis by 2025 by aggressively implementing new disease control strategies. The program includes enhancing disease surveillance, reporting, and treatment; strengthening the role of state governments; providing nutritional support to patients; compensating private medical providers for successful management of TB patients; and investments to prevent other respiratory diseases that make people more susceptible to TB. India has the world’s highest burden of TB disease, with approximately 2.8 million new cases and 420,ooo deaths in 2016. [Huffington Post; Money Control; Business Standard]
Single oral dose of cholera vaccine can be valuable in some situations. A study in Bangladesh, where cholera is endemic, showed that a single dose of Oral Cholera Vaccine (OCV) was effective in people over age five for at least two years. A two-dose series is the norm, but the study found that in disaster-hit areas where providing second doses is particularly challenging, a single dose offers protection for two or more years in older children and adults. [Lancet Infectious Diseases Article, Lancet Comment]
Bacteriophage from pond conquers tough resistant bacteria: A patient in the US survived heart valve surgery, but a subsequent drug-resistant infection could have killed him—if not for an experimental phage treatment. A team at Yale tested the in vitro efficacy of several antibiotics and a bacteriophage (OMKO1—isolated from a pond in Connecticut) against a culture of the patient’s Pseudomonas aeruginosa The phage was able to significantly reduce bacterial density in the culture, whereas the antibiotics alone did not. Researchers received approval from the FDA to use the phage as an emergency investigational new drug, and successfully eliminated the infection after just one application. [Evolution, Medicine, and Public Health, Yale News]
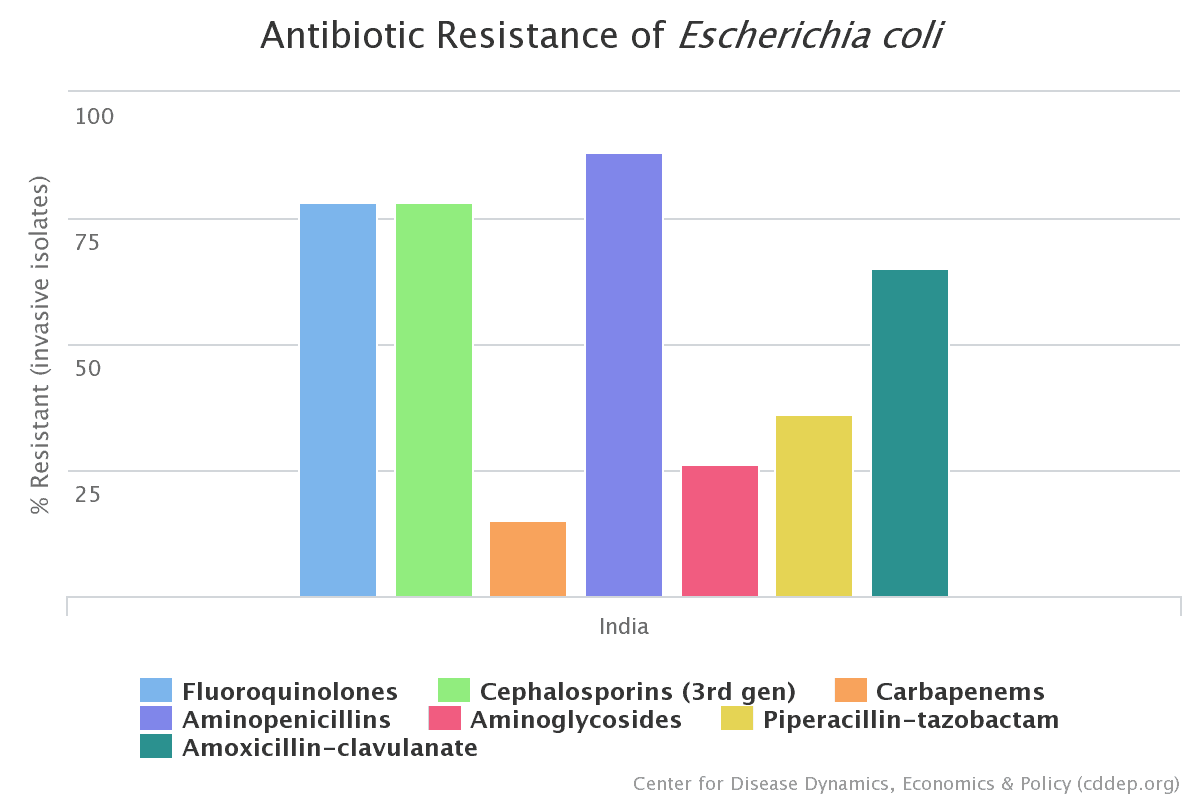
High carriage rates of resistant E-coli in children in northeastern India. Using standard antibiotic susceptibility testing, researchers studied fecal isolates from the stool of children aged 1 to 14. They found that prevalence of resistance to ampicillin was highest at 92%, followed by ceftazidime (90%), cefoxitin (88%), streptomycin (40%), and tetracycline (36%). These rates are similar to national rates for India on ResistanceMap. [BioRxiv]
Moral values of purity and liberty count more than fairness in decision making of vaccine doubters. Seeking to understand anti-vaccine parents in the United States, researchers conducted a study based on Moral Foundations Theory, using a framework that quantifies how strongly the values of authority, care (cherishing and protecting others), fairness, liberty, loyalty, and purity influence vaccination decisions. High-hesitancy respondents were twice as likely to strongly emphasize purity relative to low-hesitancy respondents. Campaigns designed to appeal to purity and liberty might be more likely to be compelling to vaccine-doubting parents than campaigns based on fairness and care. [Scientific American, Nature Human Behavior ]
Prescribers have not heeded calls to reduce outpatient antibiotic use in the US. A study published in Infection Control & Hospital Epidemiology has found that current initiatives to improve the use of antibiotics in outpatient settings may not be enough to change clinicians’ prescribing practices. Public health initiatives and new guidelines made no dent in the massive number of antibiotic prescriptions—nearly 33 million—filled in the US each year. MedicalXpress, Infection Control & Hospital Epidemiology]
New molecules doing new tricks: A new class of synthetic polycarbonates has prevailed against numerous drug-resistant bacteria in mice. Scientists found that their guanidinium-enhanced polymers were able to destroy five resistant bacterial infections (Acinetobacter baumannii, Escherichia coli, Klebsiella pneumoniae, MRSA, and Pseudomonas aeruginosa). The new molecule loses bioactivity when it disintegrates (after 72 hours in the body), is non-toxic to human cells, and (thus far) does not induce drug resistance in its targets. The international research team, a joint effort of IBM Research (US) and the Institute of Bioengineering and Nanotechnology (Singapore), says they are ready to proceed with human trials. [Nature, Plastics News, Popular Science]
Scientists unravel Typhoid bacteria mutation causing XDR outbreak in Pakistan. Genes causing resistance to five antibiotics have been discovered in the bacteria responsible for over 300 extensively drug resistant cases of disease in Sindh, Pakistan (and one travel-associated case in the UK) since November, 2017. Specimens of Salmonella enterica serovar Typhi (S. typhi) from the outbreak were analyzed by a team at the Wellcome Institute and found to have remarkable genetic similarity. The bacteria’s DNA included a plasmid that may have been transferred initially from a resistant strain of coli. [Cambridge Independent, Mbio]
Reducing antibiotic overuse in rural China. A large trial in rural China tested the effects of an educational intervention on the rate at which pediatric patients were prescribed antibiotics for upper respiratory symptoms. Clinicians received guidelines and training on appropriate prescribing, attended monthly review meetings where their prescribing rates were assessed, and were provided educational materials to give to caregivers. The study found that the intervention led to an absolute risk reduction in antibiotic prescribing of 29 percent. [Lancet Article, Lancet Correspondence, Lancet Correspondence]
MDR-TB: One-size-fits-all versus individualized treatments—can a fair balance be found? Standardized treatment regimens are the norm in low-resource settings, but such treatment is only 50% effective in patients with drug resistant TB, and suboptimal treatments can amplify resistance, which is transmissible. Standardized regimens can also cause debilitating side effects in some patients. Precision medicine guided by drug susceptibility testing can lead to improved individualized outcomes, but requires more time and infrastructure as well as more highly trained personnel. The authors of this Lancet Personal View lay out the rationale for the highest possible standard of care in each setting, addressing both ethical and practical
Humor wins antibiotic resistance film competition The Australian non-profit NPS MedicineWise recently joined forces with American Express Open Air Cinemas in a “Preserve the Power” film contest to help people understand antibiotic resistance. The winning piece, a 30-second video called “Keep the Bugs Outta the Club,” earned the winners AU$5,000 plus a pound of appreciation from people fighting antibiotic resistance around the globe. [NPS MedicineWise, YouTube]
Image Credit: CDDEP











