March 12, 2019
Uganda releases AMR National Action Plan. The Republic of Uganda released its signed Antimicrobial Resistance National Action Plan (AMR NAP) for 2018 through 2023. The action plan was developed with assistance from CDDEP’s Global Antibiotic Resistance Partnership (GARP) and the Ugandan National Academy of Sciences and includes five strategic interventions to promote public awareness for AMR, improve infection prevention and control, promote appropriate access to and use of antimicrobials, implement AMR surveillance, and invest in research and innovation. The NAP also includes implementation and monitoring and evaluation plans. [Uganda AMR NAP, CDDEP]
AMR’s role elevated at WHO. The World Health Organization’s (WHO’s) Director General, Dr. Tedros Adhanom, announced his appointments for his new senior leadership team who will work under him to implement the Thirteenth General Program of Work for 2019 to 2023. Under the reorganization, AMR’s role has been elevated to a separate pillar under the leadership of Dr. Hanan Balkhy, ADG. [WHO, Devex].
Over 200 confirmed measles cases in the US in 2019. Between January 1 and February 28, 2019, there were 206 cases of measles confirmed in 11 US states, the Centers for Disease Control and Prevention (CDC) announced. States with confirmed cases include California, Colorado, Connecticut, Georgia, Illinois, Kentucky, New Jersey, Oregon, Texas, and Washington. Six outbreaks have also been reported in 2019 in Washington, Texas, Illinois, and several across New York state. The majority of those who contracted measles were unvaccinated and many cases were linked to international travel. [CDC]
MSF suspends Ebola response activities in Katwa, DRC. Médecins Sans Frontières (MSF) suspended all activities at an Ebola treatment center in Katwa, Democratic Republic of Congo (DRC) following a violent attack that destroyed several medical wards and equipment and reportedly resulted in the death of one person, the international organization stated in a press release. MSF personnel and patients were evacuated from the facility. [MSF]
Philippines revokes Sanofi’s dengue vaccine license. The Philippines Food and Drug Administration halted all sales, distribution, and marketing of Sanofi’s dengue vaccine, Dengvaxia, because the company failed to comply with post-marketing authorization, Reuters reported. Product registration for Dengvaxia was suspended in December 2017, and a criminal investigation was opened after Sanofi announced the vaccine could increase the risk of severe disease in unexposed children. [Reuters]
Atovaquone on mosquito nets kills malaria parasite. Exposing female Anopheles gambiae mosquitoes to low concentrations of the antimalarial atovaquone on treated surfaces such as mosquito nets blocks the life cycle and prevents the transmission of Plasmodium falciparum parasites that cause malaria. Atovaquone, and other cytochrome b inhibiting-compounds, interfere with the parasite’s mitochondrial function preventing development when the mosquitoes are exposed to the antimalarial before or shortly after P. falciparum infection. Lacing mosquito nets with atovaquone or similarly effective antimalarials may help eradicate malaria especially in the age of growing insecticide resistance, researchers noted. [Nature]
UK primary care physicians prescribe longer antibiotic courses than recommended in clinical guidelines. Researchers reviewed data from the UK’s Health Improvement Network to understand antibiotic prescribing in primary care for 13 common infections, including acute sinusitis, acute sore throat, acute cough and bronchitis, and pneumonia, among others. Between 2013 and 2015, 931,015 primary care office visits for the selected infections resulted in antibiotic prescriptions. Prescribed durations exceeded recommended guidelines by 1.3 million days in total. Over 80 percent of antibiotic treatments for upper respiratory tract infections exceeded guideline recommendations. [BMJ]
Variability in antibiotic prescribing for kids in European emergency rooms. Between November 2014 and February 2016, researchers enrolled 5,177 children aged 1 month to 16 years who presented with fever to one of 28 European emergency departments into an observational study to assess variability in antibiotic prescribing practices. Of the 4,560 children without comorbidities, 32 percent were prescribed antibiotics, and 61 percent of these prescriptions were for second-line antibiotics. The majority of antibiotics were prescribed for respiratory tract infections. Antibiotic prescribing rates varied from 19 percent in Switzerland to 64 percent in Turkey. [The Lancet Infectious Diseases]
Prevalence of C. difficile infections associated with antibiotic use in US and Brazil. Between 2006 and 2012, the annual rate of hospital-onset Clostridium difficile infection (HO-CDI) across more than 500 acute care hospitals in the US was 7.3 per 10,000 patient-days. Increased antibiotic use was associated with higher rates of HO-CDI; for every 50 days of therapy per 1,000 patient-day increase in total antibiotic use, there was a 4.4 percent increase in HO-CDI, according to a cross-sectional analysis. In a separate study, researchers assessed CDI prevalence among 6,374 patients, aged 18 years or older, who were admitted to one of eight university hospitals in Brazil. Over the two-day study period, the prevalence of CDI was 3.0 per 1,000 patient days, and exposure to fluoroquinolones was associated with increased risk of infection with a relative risk of 3.13 compared to those who did not take fluoroquinolones. [CID, ICHE]
ESBL-E carriage common among neonates admitted to Kenyan hospital. Between July 2013 and August 2014, the at-admission prevalence of extended-spectrum β-lactamase–producing Enterobacteriaceae (ESBL-E) carriage among 569 neonates admitted to Kilifi County Hospital’s high-dependency unit or general pediatric ward was 10 percent. Delivery by cesarean section, older neonatal age, and smaller household size were significant risk factors for at-admission ESBL-E carriage. An additional 55 percent of admitted neonates acquired carriage during their hospital stay, and the acquisition rate was 21.4 percent per day. Most ESBL-E isolates were multidrug resistant and commonly demonstrated resistance to chloramphenicol, trimethoprim-sulfamethoxazole, quinolones, and gentamicin. [CID]
Electronic ordering intervention reduces unnecessary urine culture tests and cuts lab costs. Implementation of an electronic physician order entry system for urine culture reflex tests was associated with a 45 percent reduction in the number of urine cultures ordered at a tertiary care facility in the US. Before the intervention, from January 2015 to April 2016, the clean catch urine culture rates were 30 cultures per 1,000 patient days and the catheterized culture rates were 7.8 per 1,000 patient days. Following the intervention, from May 2016 to August 2017, those rates fell to 18.7 and 1.9 cultures per 1,000 patient days, respectively. The proportion of positive urine cultures increased from 25.5 percent to 29.7 percent post-intervention, and the reduction of unnecessary urine culture ordering resulted in a $6,490 reduction in monthly laboratory costs. [ICHE]
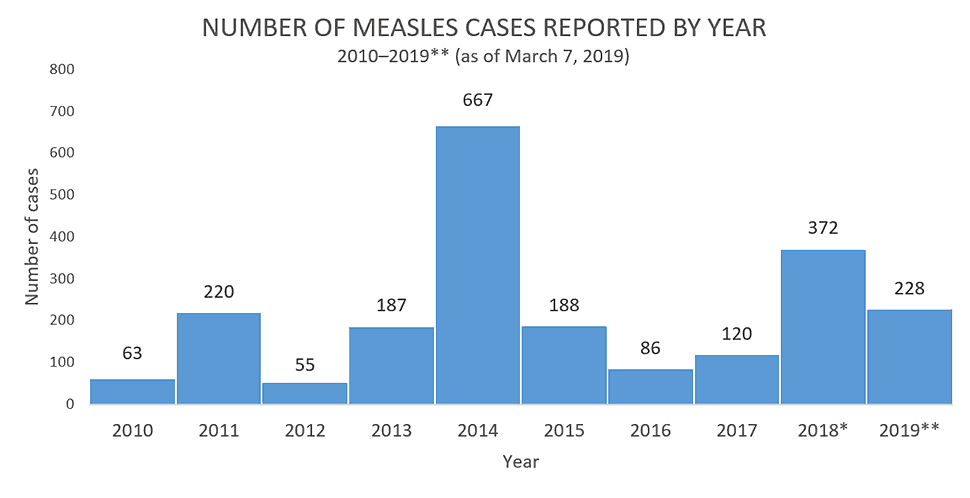
Photo: Number of Measles Cases Reported by Year: 2010-2019 (as of March 7, 2019). Source: CDC.











