November 02, 2018
Report examines link between primary health care and AMR. CDDEP research presented at the Global Conference on Primary Health Care identifies challenges and opportunities to address antimicrobial resistance (AMR) in primary health care facilities in low- and middle-income countries. Ineffective first-line antibiotics, lack of access to improved sanitation facilities, and staff who are undertrained in proper antimicrobial usage may help spur AMR. Strategies to mitigate AMR in the primary health care setting include: developing national action plans that account for the central role of primary health care providers in tackling AMR and implementing comprehensive community-based monitoring systems to track antibiotic consumption. Improvements in primary health care are instrumental in increasing access to affordable care and reducing misuse of antimicrobials. [Report]
FDA approves a single-dose, fast-acting flu drug. The US Food and Drug Administration (FDA) has approved a new fast-acting influenza drug, Xofluza, that can be taken in a single oral dose. In clinical trials, Xofluza alleviated symptoms in a shorter period compared to other flu treatments when taken within 48 hours of symptom onset. The FDA approved the drug for individuals aged 12 years and older. [FDA, STAT News, CNN]
Maternal mortality, stillbirths, and neonatal deaths in South Asia and sub-Saharan Africa. Researchers with the Alliance for Maternal and Newborn Health Improvement conducted a prospective cohort study in 11 community-based sites in South Asia (SA) and sub-Saharan Africa (SSA) and collected outcome data for over 250,000 pregnancies. Overall, maternal mortality rates were similar for SA and SSA with rates of 336 and 351 per 100,000 live births, respectively. Leading causes of maternal mortality and stillbirths were obstetric hemorrhage, non-obstetric complications, hypertensive disorders, and pregnancy-related infections. Stillbirth rates were 35.1 and 17.1 per 1,000 births in SA and SSA, respectively. Neonatal death rates were 43.0 and 20.1 per 1,000 livebirths in SA and SSA, respectively, and leading causes of neonatal deaths were perinatal asphyxia, severe neonatal infections, and complications of preterm birth. [The Lancet]
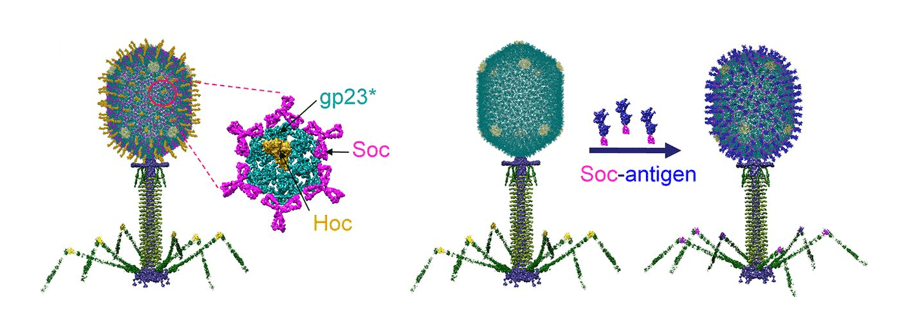
New vaccine protects against inhalational anthrax and pneumonic plague. Researchers have developed a vaccine that protects against both anthrax and pneumonic plague by using viral antigen nanoparticles and a bacteriophage T4 platform to elicit an immune response. In animal model studies, the vaccine provided 100 percent protection against anthrax and plague when the viruses were administered sequentially. When mice were simultaneously exposed to lethal doses of both anthrax and plague, the vaccine provided 88 percent protection. [mBIO, Newsweek]
Despite progress in antibiotic prescribing, antibiotic-resistant superbugs remain a threat in England. Between 2014 and 2017, total antibiotic consumption in England decreased by 6.1 percent, Public Health England (PHE) reported in its annual publication on antibiotic use, resistance, and stewardship. Between 2013 and 2017, there was a 13.2 percent drop in antibiotic prescriptions in the primary health care setting, where the majority of antibiotic prescriptions are dispensed. In that same timeframe, the proportion of blood culture isolates of Escherichia coli, Klebsiella pneumoniae, and other enterococci resistant to key antibiotics remained stable which is likely a reflection of improved antimicrobial stewardship efforts. However, the total number of bloodstream infections caused by a pathogen resistant to one or more antibiotics increased by 35 percent from 12,250 in 2013 to 16,504 in 2017. [PHE, The Telegraph]
Spread of mutation-harboring multidrug-resistant TB undetected by WHO-endorsed diagnostics. In a South African study, 37 of 249 (15 percent) Mycobacterium tuberculosis (TB) samples had a rpoB gene mutation that confers resistance to first-line TB drugs including isoniazid, pyrazinamide, and ethambutol. Two molecular assays endorsed by the World Health Organization (WHO) for the rapid diagnosis of TB failed to identify the rpoB gene mutation. This diagnostic gap and a lack of surveillance leads to inappropriate first-line treatments and undetected spread of TB strains harboring this mutation. [The Lancet Infectious Diseases]
Rubella outbreak in Japan. An ongoing rubella outbreak in Japan has infected over 1,000 people so far in 2018 and has prompted the US Centers for Disease Control and Prevention (CDC) to issue a travel alert for the country. Most recent cases have been reported in the Kanto region which includes Tokyo. The CDC advises travelers to Japan, particularly pregnant women, ensure they are vaccinated or otherwise protected against rubella. [NIID, CDC, The Japan Times, The Mainichi]
Chinese drug company fined billions of yuan for faulty rabies vaccines. Changchun Changsheng Biotechnology, a Chinese drug company, was fined 12 million yuan, or US $1.7 million, by national and local agencies for using expired ingredients and failing to properly test the potency of several batches of rabies vaccines. The company’s license to make rabies vaccines was revoked, and 14 of its executives have been banned from working in the pharmaceutical sector. [Nature]
Multidrug-resistant gonorrhea on the rise. In many high-income countries, current clinical guidelines for the treatment of Neisseria gonorrhoeae infections recommend a dual drug regimen of ceftriaxone and azithromycin. This treatment paradigm is losing efficacy as multi-drug resistant N. gonorrhoeae strains emerge worldwide. In 2017, sustained spread of ceftriaxone-resistant N. gonorrhoeae strains was reported in five countries. In 2018, strains with dual resistance to ceftriaxone and azithromycin were reported in the United Kingdom and Australia. In response, the World Health Organization has called for increased antimicrobial resistance surveillance and researchers recommended additional research to assess the threat and impact of multidrug-resistant N. gonorrhoeae. [The Lancet]
Poor diagnostic ability associated with inappropriate antibiotic prescriptions in rural China. Researchers from the US and China randomly sampled over 300 township health centers and village clinics from three provinces in China to examine inappropriate antibiotic prescribing in the primary health care setting. Overall, antibiotics were inappropriately prescribed to 42 percent of patients. Inappropriate prescribing was linked with diagnostic ability as providers who made a correct diagnosis were less likely to prescribe antibiotics compared with those who made incorrect diagnoses. [Journal of Antimicrobial Chemotherapy]
Immigration to the US associated with immediate changes to gut microbiome. A new study assessed the impact of US immigration on gut microbiome composition. Researchers compared microbiome diversity among Hmong and Karen women who were living in Thailand to women of the same ethnic groups who immigrated to the US or who were born in the US. Hmong and Karen women living in Thailand had the most diverse microbiomes. Microbial diversity was lower among women who immigrated to the US and continued to decline as duration of residence in the US increased. Moreover, immigrants living in the US for more than a decade were more likely to be obese, and lower microbiome diversity was associated with obesity. [Cell, The Atlantic, NPR]
Please note that CDDEP will not publish a Weekly Digest next week (November 5-9) due to Diwali holidays.
Image: Schematic of the bacteriophage T4 nanoparticle platform used in new vaccine for inhalation anthrax and pneumonic plague. Tao et al. (CC 4.0)











