November 11, 2019
Vaccine protects against tuberculosis progression. According to a 3-year analysis of tuberculosis-infected patients in Kenya, South Africa, and Zambia, a candidate TB vaccine (M72/AS01E) provided 49.7 percent protection against active pulmonary TB disease. Incidence of active pulmonary TB was 0.3 cases per 100 person-years in the vaccine group compared to 0.6 cases per 100 person-years in the placebo group. The vaccine showed sustained immunogenicity for the full 36-month follow-up, and frequency of serious adverse events and deaths occurred equally across vaccine and control groups. [NEJM]
Most US restaurant chains receive failing grades for antibiotic use in beef. The Chain Reaction V report, which rates the top 25 major restaurant chains in the United States on antibiotic use in their meat, indicates that a majority receive failing grades for the routine use of medically important antibiotics in beef. Chipotle and Panera received ‘A’ grades for their responsible use of antibiotics, while Burger King, Sonic, Applebee’s, Arby’s, Chili’s, and Buffalo Wild Wings among others received failing grades. McDonald’s and Taco Bell improved to “C” and “D” grades this year as a result of new commitments to responsible antibiotic use in their beef. The companies were scored on policy, implementation, and transparency around antibiotic use across their meat supply chains. [NRDC]
CDC notes reduction in various healthcare-associated infections. The US Centers for Disease Control and Prevention (CDC) released the 2018 National and State Healthcare-Associated Infections (HAI) Progress Report, which notes a reduction in various incident HAIs in the United States in 2018, as well as areas for improvement. The CDC reports an overall decrease in central line-associated bloodstream infections, catheter-associated urinary tract infections, and hospital-onset C. difficile infections between 2017 and 2018 (9, 8, 12 percent reductions, respectively). Compared to 2017, 20 states performed better on at least two infection types in acute care hospitals in 2018, while two states performed worse. There were no significant overall changes in ventilator-associated events, surgical site infections, or hospital-onset methicillin-resistant Staphylococcus aureus (MRSA) bloodstream events between 2017 and 2018. [CDC]
Measles may cause long-term damage to children’s immune systems. A study in Science analyzed the immune systems of unvaccinated children before and after infection with measles compared to the immune systems of vaccinated children. Children with severe and moderate measles lost a median of 40 and 33 percent of their pre-existing pathogen-specific antibody repertoires, respectively. Vaccinated children who were not infected with measles retained ~90 percent of their antibody repertoires. The study provides the first biological evidence of long-term immune system damage following measles, and may explain the increase in child morbidity and mortality that lasts up to 5 years after measles infection. [Science]
TB Alliance partners with manufacturer in India to produce resistant TB drug. TB Alliance, a non-profit drug developer, announced its partnership with Macleods Pharmaceuticals Limited, a generic manufacturer in India, to produce pretomanid for the treatment of extensively drug-resistant tuberculosis (XDR-TB). Macleods will commercialize the drug in 140 countries with high TB incidence. [TB Alliance]
Proportion of countries with school-based vaccination increases slightly. A global analysis of school-based vaccination noted a slight increase in the percentage of countries that reported school-based delivery of at least one routinely recommended vaccine, from 58 percent of countries in 2008 to 60 percent in 2017. Tetanus, diphtheria, and human papillomavirus (HPV) were the most common vaccines delivered through school settings in 2017. [Vaccine]
New details released about patients who contracted resistant infections from fecal transplants. New details have been released regarding the two patients who were exposed to extended-spectrum beta-lactamase (ESBL)-producing Escherichia coli bacteremia following fecal microbiota transplantation (FMT) earlier this year; one of whom died. The two patients were enrolled in FMT trials at Massachusetts General Hospital and became sick 8 and 17 days following FMT procedure. The two patients received stool from the same donor, which was not screened for ESBL-producing pathogens prior to the transplantation. In January 2019, Massachusetts General expanded stool screening to include ESBL-producing pathogens, but existing inventory was not re-screened. [NEJM]
Quality improvement program improves antimicrobial stewardship in NICUs. Researchers evaluated the implementation of CDC core elements for antimicrobial stewardship across 146 neonatal intensive care units (NICUs) that participated in an internet-based quality improvement (QI) collaborative between 2016 and 2017. Results showed an overall increase in all of the CDC core elements, including leadership, accountability, drug expertise, actions, tracking, reporting, and education. The median rate of antibiotic use among newborns also decreased significantly following the QI collaborative, from 16.7 to 12.1 percent. [Pediatrics]
Over-the-counter antibiotic dispensing lower in Udupi than other regions in India. Researchers conducted 1522 standardized patient interactions at 279 pharmacies in Udupi district, India to measure over-the-counter antibiotic dispensing. Antibiotics were dispensed in 4.34 percent of adult patient interactions and 2.89 percent of child patient interactions where an adult acted as a proxy. These dispensing rates are substantially lower than rates reported in other regions in India. A greater number of questions asked and longer patient-pharmacist interactions were linked to increased odds of antibiotic dispensing (OR=1.54, 3.03), while referral to another provider was linked to decreased odds of antibiotic dispensing (OR=0.38). [BMJ Global Health]
Global trends and risk factors of under-5 deaths from lower respiratory infections. An analysis of data from the Global Burden of Diseases, Injuries, and Risk Factors Study identified a 65.4 percent decrease in under-5 deaths from lower respiratory infection (LRI) between 1990 and 2017. Increased coverage of Haemophilus influenza type b vaccination, increased converge of pneumococcal vaccination, and reductions in household air pollution contributed to the greatest decrease in under-5 LRI mortality during the study period. [The Lancet Infectious Diseases]
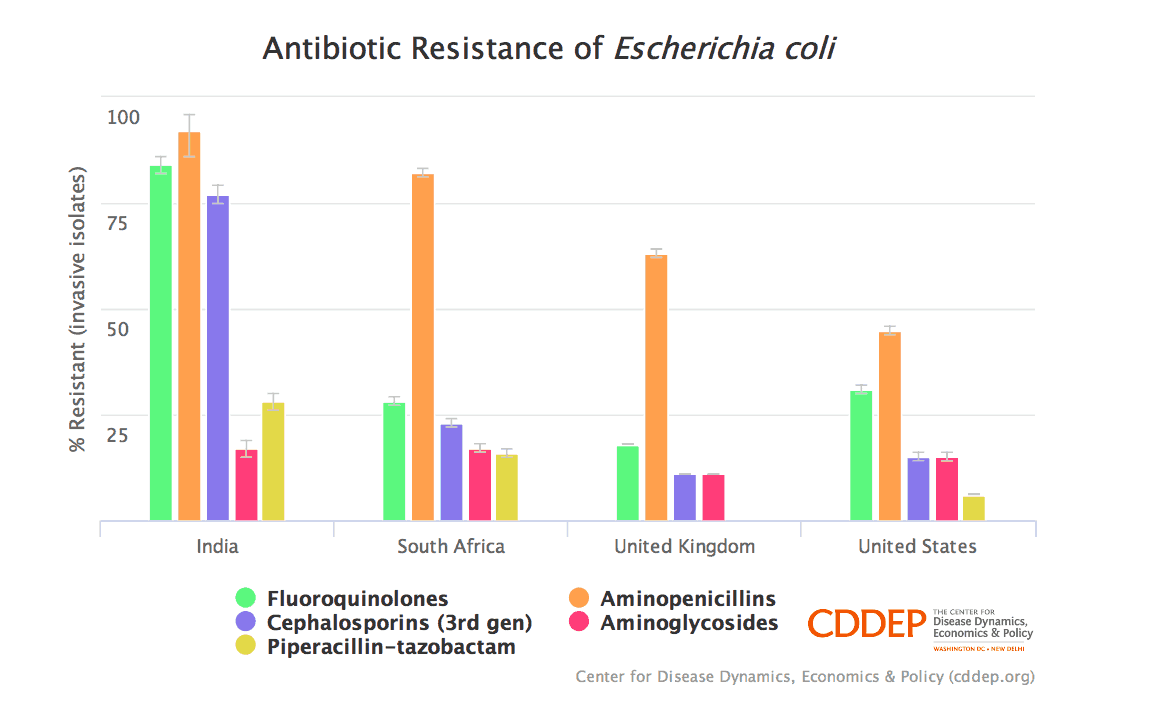
Antibiotic resistance of E. Coli in India, South Africa, UK, and the US. [CDDEP]