October 14, 2019
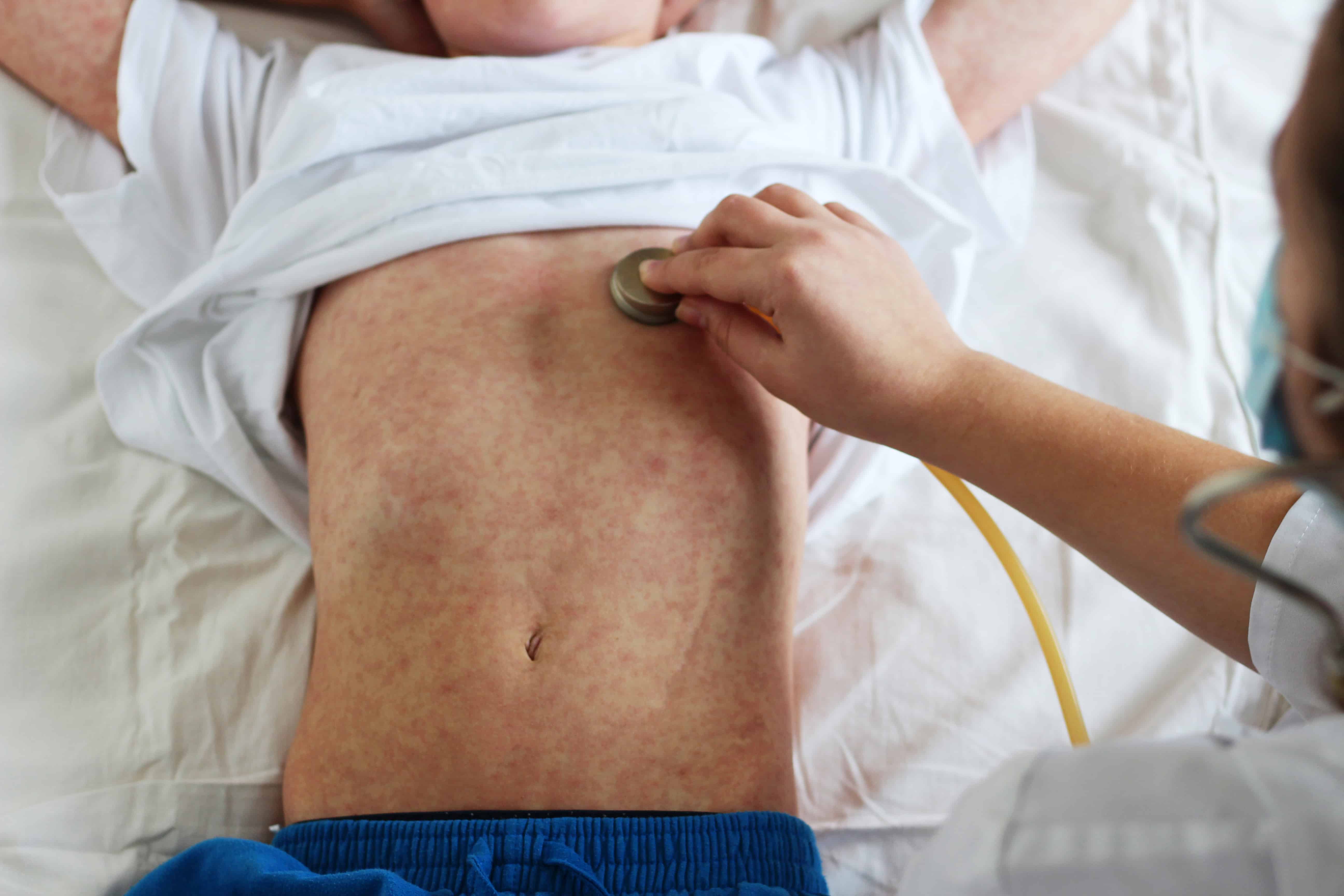
Vaccine-hesitant communities drive US measles outbreak. The US Centers for Disease Control and Prevention (CDC) released a national measles update, stating that 1,249 cases were reported between January and September 2019. This is the highest annual case count since 1992. Almost 90 percent of 2019 US measles cases occurred in close-knit, vaccine-hesitant communities, and Orthodox Jewish communities in New York accounted for 75 percent of cases. [MMWR]
Poultry raised with antibiotics more likely to be contaminated with resistant pathogens. Researchers reviewed chicken and turkey samples purchased in Pennsylvania and found that nearly twice as many samples from conventionally raised poultry were contaminated with multidrug-resistant Salmonella compared to samples from antibiotic-free poultry (10.2 vs. 5.3 percent). Salmonella found in meat that was raised with antibiotics was also more likely to be resistant to three or more antibiotics compared to antibiotic-free meat (55 vs. 28 percent). [IDSA]
High prevalence of antibiotic resistance genes found in groundwater. Researchers in Southern California analyzed levels of antibiotic resistance genes in water samples from an advanced groundwater treatment facility and groundwater aquifers. The advanced groundwater treatment facility filtered out a majority of the targeted antibiotic resistance genes to below detection limits (<50 copies/L), but genes that conferred resistance to sulfonamides and β-lactams were highly prevalent in groundwater samples collected from control locations as well as locations recharged with water from the water treatment facility. [Environmental Science and Technology Letters]
Resistant UTIs are increasing among older patients in the US. In a national retrospective study using US hospital data, researchers from Queen’s University Belfast found that the proportion of older patients with antibiotic-resistant urinary tract infections (UTIs) increased from 3.64 to 6.88 percent between 2009 and 2016. Resistant infections were associated with discharge into a care facility (OR=1.81), longer hospital stays (1.12 days), and increased hospital costs ($1259 USD). Methicillin-resistant Staphylococcus aureus (MRSA) was also associated with an increase in hospital mortality (OR=1.33). [PLOS ONE]
Non-prescription antibiotic dispensing is decreasing but still common in Chinese pharmacies. Using a simulated client method in nearly 2500 community pharmacies across six provinces in China, researchers observed non-prescription antibiotic dispensing during 48.5 percent of pediatric diarrhea simulations and 70.1 percent of adult upper respiratory tract infection simulations. Non-prescription antibiotic dispensing was more common in rural areas compared to urban, and was inversely associated with the presence of an onsite pharmacist (OR= 0.66). Trends in non-prescription antibiotic prescribing decreased significantly in Shaanxi province between 2011 and 2017, from 72.3 to 50.2 percent of pediatric cases and from 95.8 to 69.5 percent of adult cases. [The Lancet Infectious Diseases]
Drug resistance and mortality are high among patients with A baumannii pneumonia. Researchers from Malaysia and Australia compiled results from 126 studies spanning 29 countries and identified a 42.6 percent pooled mortality rate among patients with Acinetobacter baumannii causing hospital-acquired and ventilator-associated pneumonia. The prevalence of multidrug-resistance in Acinetobacter baumannii pneumonia was 79.9 percent. Prevalence was highest in Central America and Latin America/Caribbean and lowest in Eastern Asia (100 percent vs. 42.6 percent, respectively). [Journal of Infection]
Nearly 80% of pre-appointment dental antibiotics are prescribed unnecessarily. According to a study presented at ID Week 2019 in Washington, DC, 80 percent of antibiotics prescribed before dental visits between 2011 and 2015 in the US were unnecessary, according to current American Dental Association and American Heart Association guidelines. Unnecessary dental antibiotic prescribing led to nearly 4,000 allergic reactions, 1568 visits to the emergency room, and 9 Clostridioides difficile infections. [IDSA, CIDRAP]
Antibiotic use and length of hospital stay are unaffected by rapid viral testing. A randomized controlled trial involving nearly 1000 adults with respiratory symptoms or other acute care conditions in Finland found that the use of rapid viral testing did not have an effect on antibiotic use or length of hospital stay among patients. The intervention group received viral test results within 24 hours, while the control group received results within one week. The difference in length of hospital stay and days on antibiotics between the two groups was insignificant (mean difference: 0.1, 0.9, respectively; p=0.810, 0.235). [Clinical Microbiology and Infection]
Fear acts as a barrier for participation in vaccine trials. Results of a survey among five clinical research sites in France identified common barriers and motivators for participating in preventive vaccine trials (PVT). Respondents who agreed to participate in a PVT were more likely to be younger, involved in early phase vaccine trials, more educated, and have a more positive/favorable opinion towards vaccines compared to those who denied participation. Fear of vaccine side effects was one of the most common barriers to PVT participation, and was noted by 36.6 percent of respondents who denied participation. Results suggest that increasing vaccine hesitancy may make PVT recruitment progressively difficult. [Vaccine]
Malaria chemoprevention reduces infections in children. In a clinical trial, investigators found that seasonal malaria chemoprevention was associated with fewer malaria episodes in children, lower fold changes in CD4+PD1+ and CD4+PD1+LAG3+, and greater increases in CD4+FOXP3+ T regulatory cells compared to those that did not receive chemoprevention. Results of the trial suggest that the effects of seasonal malaria chemoprevention could prevent immune dysfunction among children as well. [Journal of Infectious Diseases]
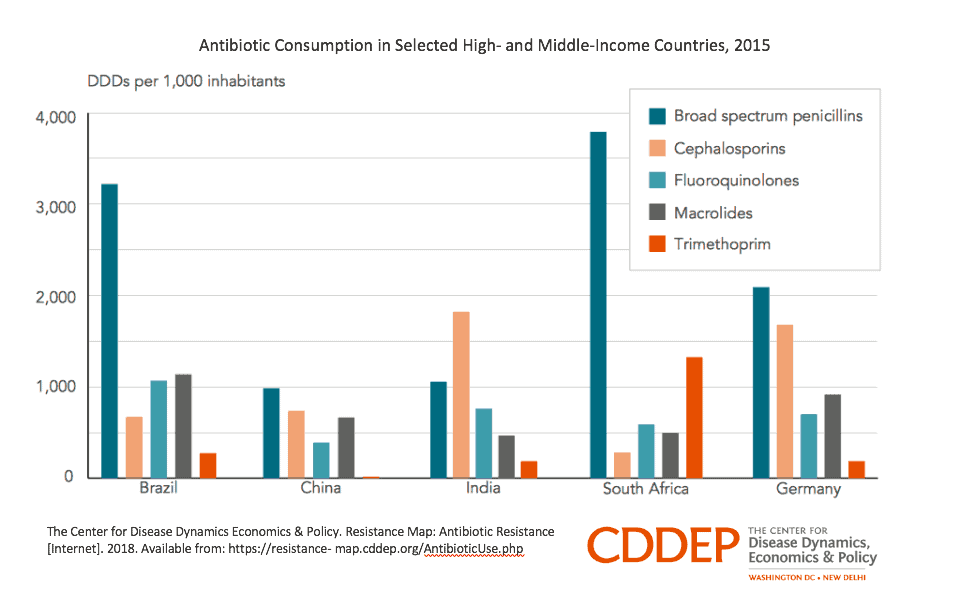
Antibiotic consumption in selected high- and middle-income countries in 2015. [CDDEP]