October 07, 2019

Antibiotic stewardship programs now required in US hospitals. The Centers for Medicare and Medicaid Services (CMS) finalized a new rule that will require all US hospitals and critical access hospitals to implement antibiotic stewardship and infection prevention and control programs within 6 months in order to receive CMS reimbursements. The rule was initially proposed in June 2016. [CMS]
Brazil and US lead measles case counts in the Americas. According to the Pan American Health Organization, 14 countries and territories in the Americas have reported confirmed measles cases in 2019 to date. A total of 6,541 cases, including 5 deaths, have been documented, with Brazil (4,476 cases) and the United States (1,241) accounting for 87 percent of all measles cases in the region. While the US reported 69 additional cases between August and September (compared to 205 between May and June), Brazil noted 3,431 additional cases of measles within the same period (compared to 49 between May and June). [PAHO]
GARDP funds phase 3 trial of novel antibiotic for uncomplicated gonorrhea. The Global Antibiotic Research and Development Partnership (GARDP) and Entasis Therapeutics have launched a randomized phase 3 trial for zoliflodacin, a novel antibiotic for the treatment of uncomplicated gonorrhea. Approximately 1,000 adults with urogenital gonorrhea across four countries (the United States, the Netherlands, Thailand, and South Africa) will be enrolled in the trial, and researchers will assess the efficacy and safety of the antibiotic against the current standard of care. [GARDP]
Multiple-bed hospital rooms non-inferior to single-bed rooms as a contact precaution for resistant bacteria. A cluster-randomized study of 16 Dutch hospitals found multiple-bed hospital rooms non-inferior to single-bed hospital rooms as a contact precaution for extended-spectrum β-lactamase (ESBL)-producing Enterobacteriaceae. In hospitals randomized to a single-bed room strategy, transmission of the bacteria from an index patient to at least one ward mate occurred for 4 percent of patients, while transmission occurred for 7 percent of patients randomized to the multiple-bed room strategy (crude risk difference: 3·4 percent, 90% CI: 0·3 to 7·1). These findings may prompt a change in the current preferred contact precaution for ESBL-producing Enterobacteriaceae. [The Lancet Infectious Diseases]
Candida auris outbreak in London cost over $1.2 million to control. According to an outbreak report from King’s College Hospital in London, a 2016 Candida auris outbreak involving 34 cases cost over $1.2 million USD to control, not including costs due to lost opportunity. Four cases died within one month of C. auris colonization or infection, and C. auris infections were linked with longer hospital stays, haemodialysis, and antifungal therapy. [Journal of Infection]
NICU washing machine acts as reservoir for drug-resistant bacteria. Between 2012 and 2013, 13 infants and one child were colonized with extended-spectrum beta-lactamase (ESBL) producing Klebsiella oxytoca ST201 in a neonatal intensive care unit (NICU) in Germany. The multidrug-resistant pathogen was linked to a washing machine that was used to wash the newborns’ laundry. The study suggests the need for improved washing machine design to prevent microbial growth, contamination, and transmission. [Applied and Environmental Microbiology]
Outpatient settings lack proper first-line antibiotic prescribing. Researchers from the US Centers for Disease Control and Prevention (CDC) and the Pew Charitable Trusts found that only 50 percent of patients who visited a US outpatient setting for pharyngitis, sinusitis, and acute otitis media in 2014 received recommended first-line antibiotics. First-line antibiotic prescribing was lowest in urgent cares (49 percent) and highest among children (62 percent). [Antimicrobial Agents and Chemotherapy]
Cholera vaccination coverage in Haiti following the first global stockpile deployment campaign. Researchers conducted a survey to evaluate departmental coverage of the oral cholera vaccine (OCV) in Haiti following the first global OCV stockpile deployment campaign targeting over 180,000 Haitians in 2014. Two-dose OCV coverage was 70 percent in Artibonite, 63 percent in Centre, and 44 percent in Ouest, and coverage was higher in children 5-14 years old than those 15 and older. The study suggests that lower coverage in Ouest may be attributable to poor social mobilization of the campaign. [Vaccine]
Mistrust and misinformation among caregivers influence childhood vaccination in Indonesia. Researchers from Australia conducted parental interviews in Tangerang Selatan, Banten Province, Indonesia to identify reasons for incomplete childhood vaccination. Caregivers of unimmunized children identified Islamic beliefs, perceived effectiveness of natural immunity, perceived benefits of alternative medicine, safety concerns, mistrust, and misinformation as reasons that influenced their decision to not vaccinate their children. [Vaccine]
Investment needed to strengthen primary health care in LMICs. In a 67-country modeling analysis, researchers from Switzerland presented measures for primary health care (PHC) investments and projected the associated resource needs in low- and middle-income countries (LMICs). An estimated additional US$200–328 billion per year is required for various PHC measures from 2020 to 2030 across the countries. On average, strengthening measures centered on public health interventions and outpatient care requires an investment of an additional $32 per capita, while PHC spending per capita needs to increase from $25 to $65 in low-income countries for improved health outcomes. Overall health workforces would need to increase from 5.6 to 6.7 workers per 1000 population. Investing in PHC interventions would bring considerable health benefits, averting an estimated 60.1 million deaths and increasing average life expectancy by 3.7 years by 2030. [The Lancet Global Health]
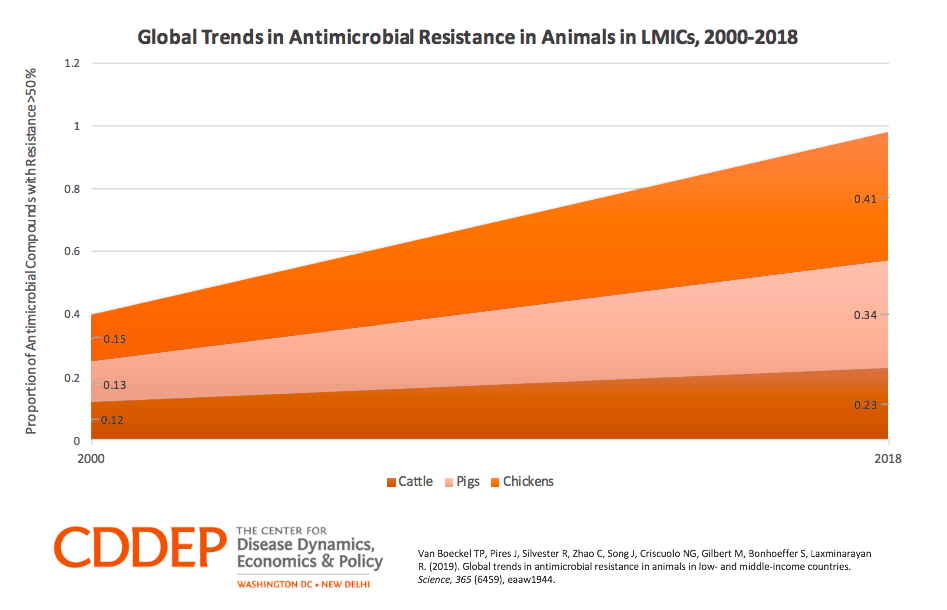
Increasing trends in antimicrobial resistance in food animals in low- and middle-income countries, 2000-2018. [CDDEP]