September 23, 2019

CDDEP researchers find increasing antibiotic resistance in food animals. Researchers from CDDEP, ETH Zurich, Princeton University, and Université Libre de Bruxelles mapped global trends in antimicrobial resistance rates among food animals in low- and middle-income countries between 2000 and 2018. The study found that the proportion of antimicrobial compounds in food animals that showed resistance higher than 50 percent (P50) increased overall between 2000 and 2018. Among the developing countries included in the study, p50 increased from 15 to 41 percent in chickens and from 13 to 34 percent in pigs, while plateauing between 12 and 23 percent in cattle. The highest rates of resistance were identified in antibiotics commonly used in food production, including tetracyclines, sulfonamides, and penicillins. Rates of resistance varied among medically important antibiotics, from 20-60 percent for ciprofloxacin and erythromycin, and 10-40 percent for third and fourth generation cephalosporins. [Science, CDDEP, WIRED, The Guardian, Times of India]
Antibiotic resistance in sewage correlates with hospital samples. A population-level observational study found a strong correlation (r2 = 0.95, 0.89 for urine and blood samples, respectively) between the rates of antibiotic-resistant Escherichia coli isolates obtained from hospital patients and hospital sewage systems in Sweden. These findings suggest that sewage systems could be a useful tool for antibiotic resistance surveillance. [Eurosurveillance]
High prevalence of resistance found in mass-transit systems around the world. Researchers collected samples from mass transit systems in 58 cities around the world over three years to map the prevalence of antimicrobial resistance (AMR) genes, and identified Latin America as a hotspot. The study team identified ten times more resistance genes among samples collected in transit systems in Rio de Janeiro and Bogotá compared to samples collected in Paris, Baltimore, or Singapore. [BioRxiv]
Bacterial infections and AMR in newborns across sub-Saharan Africa. A study of 84,534 newborns from 56 countries across sub-Saharan Africa between 2000 and 2018 found that Staphylococcus aureus accounted for 25 percent of all reported bacteremia or sepsis cases. Klebsiella spp. and Escherichia coli accounted for 21 percent and 10 percent of cases. Group B streptococcus, Streptococcus pneumoniae, and S. aureus accounted for 25, 17, and 12 percent of all meningitis cases, respectively. More than two-thirds of cases showed resistance to WHO recommended β-lactams. [The Lancet Infectious Diseases]
Superbug outbreak raises alarm in Tuscany, Italy. Superbug NDM-1 (New Delhi metallo-beta-lactamase 1) has raised alarm as it spreads throughout Tuscany, Italy. Since 2018, infections caused by NDM-1 have killed a reported 31 people in 17 different hospitals in the region, with over 31 cases reported in Pisa. NDM-1 was first reported in New Delhi, India in 2010 and is resistant to many antibiotic classes including carbapenems, which are often reserved as a last line of defense. NDM-1 can cause resistance in a range of bacteria, making it difficult to treat infections such as UTIs, sepsis, kidney infections, and pneumonia, among others. [The Local]
Antibiotic use linked to poor survival outcomes in cancer patients. Researchers in the UK studied 196 cancer patients and identified a significant association between previous broad-spectrum antibiotic therapy and poor survival and response outcomes to immune checkpoint inhibitor therapy (ICI). The study found that previous antibiotic use within 30 days of immunotherapy onset was associated with worse overall survival compared to those without previous antibiotic use (2 vs. 26 months, p<0.001), irrespective of patient tumor site, disease burden, or performance status. [JAMA Oncology]
Resistance increases in isolates from Florida dolphins. Scientists at Florida Atlantic University collected 733 pathogen isolates from 171 Bottlenose dolphins and found an 88.2 percent prevalence of resistance to at least one antibiotic. Resistance to erythromycin was the most common, found in 91.6 percent of isolates, followed by resistance to ampicillin and cephalothin, which was found in 77.3 and 61.7 percent of isolates, respectively. Overall rates of antibiotic resistance among the dolphins increased significantly between 2003 and 2015. [Aquatic Animals]
UK sees drop in antibiotic use among poultry. Due to antibiotic stewardship efforts by the British Poultry Council (BPC), the UK poultry sector has experienced an 80.2 percent reduction in the overall use of antibiotics and an 82.6 percent reduction in the use of critically important antibiotics since 2012. Despite a year-on-year increase of 12.4 percent in 2018 due to seasonal illness, the BPC has substantially reduced antibiotic use among poultry farmers. Among other stewardship activities, the BPC has stopped the use of third- and fourth-generation cephalosporins since 2012 and the use of polymyxins since 2016, as well as ending prophylactic use of antibiotics. The stewardship efforts continue to promote best practices in the UK and contribute to the ‘One Health’ model of combating antimicrobial resistance. [British Poultry Council]
Influencers of HPV vaccine uptake in young Singaporean students. Researchers conducted in-depth interviews and focus groups to identify barriers and facilitators of human papillomavirus (HPV) vaccine uptake among female students at the National University of Singapore. Barriers included lack of awareness, low perceived risk of cervical cancer, and stigma, while facilitators included health protection benefits and perceived vaccine safety and efficacy. Participants suggested increasing public awareness regarding cervical cancer to increase vaccine uptake. [Vaccine]
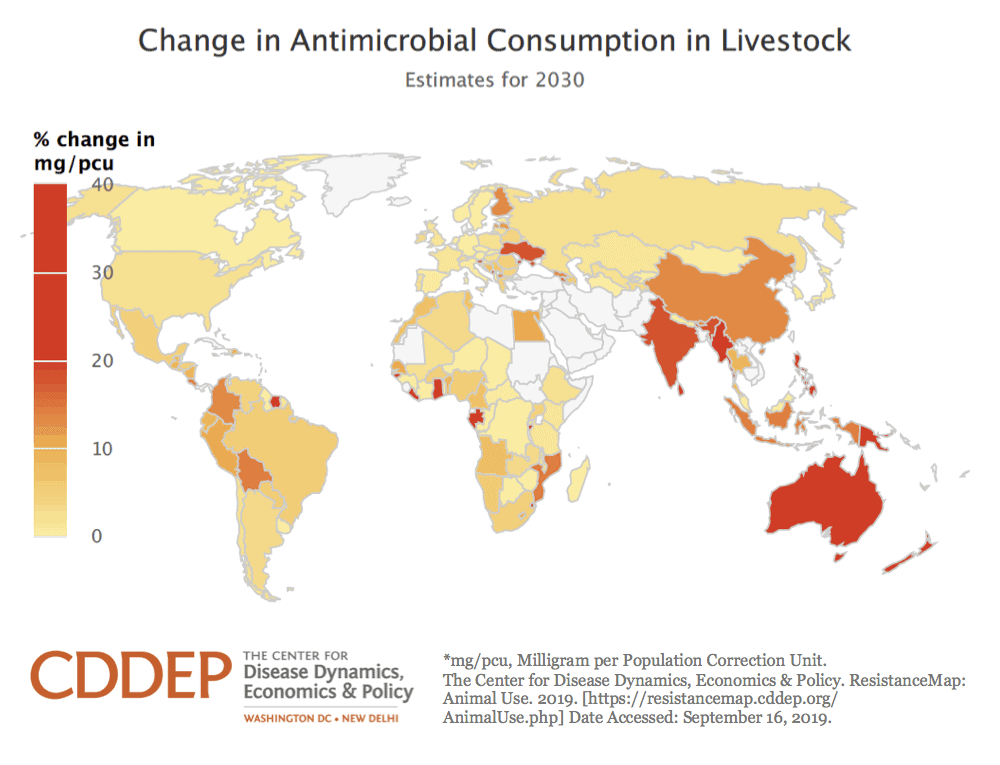
Projected changes in antimicrobial consumption by livestock in 2030. Based on current trajectories, CDDEP estimated that total antimicrobial consumption by livestock would increase by 52 percent by 2030. The main drivers will be growth in consumer demand for meat and other livestock products in middle-income countries and a consequent shift toward large-scale farming operations where antimicrobials are routinely used. [CDDEP]